ONE DOES NOT ACCUMULATE BUT ELIMINATE.
IT IS NOT THE DAILY INCREASE BUT DAILY DECREASE.
THE HEIGHT OF CULTIVATION ALWAYS RUNS TO SIMPLICITY.
—BRUCE LEE
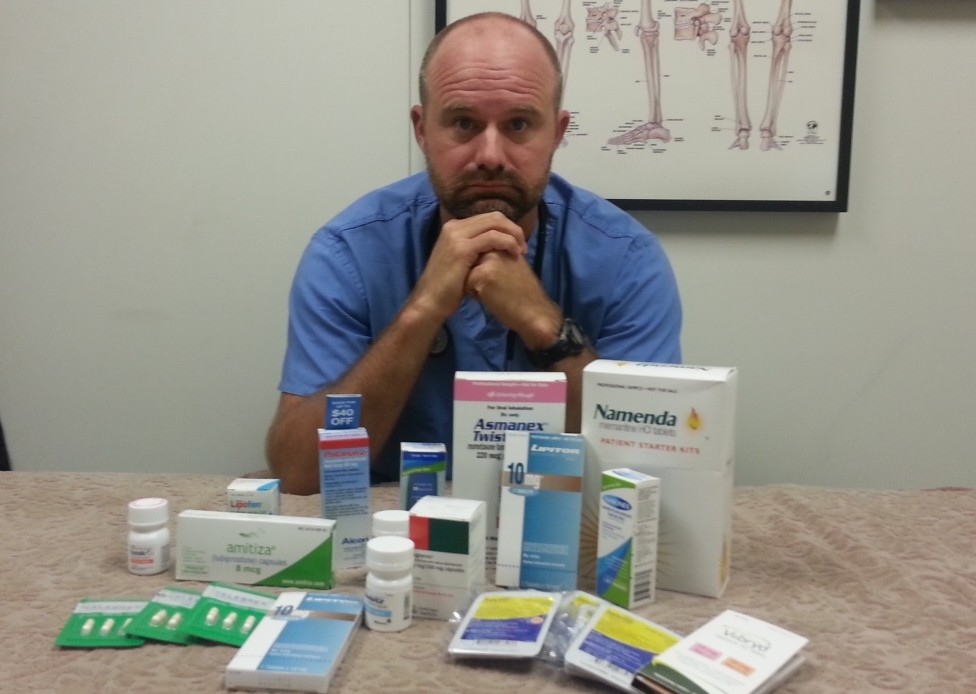
- Hazards of Poly-Pharmacy
Poly-pharmacy may for general purposes refer to the consumption of 5 or more medications concurrently; however, I was taught in medical school anything more than 3 medications carries a 100% risk of drug to drug interaction of some sort.
Everyday I see patients who have accumulated medication lists in the double digits. I am astounded when I see medication list with 13-15 medications before counting over-the-counter medications.
Unbelievable!!!
Many of these patient complain of vague conditions which defy exact cause. Not surprisingly, when I begin trimming their medication list, symptoms often abate.
Poly-pharmacy Factoids
- For every dollar medicare spends on medication, it spends $1.33 on medication related complications
- US citizens consume 80% narcotics in the world
- People > 65 years old consume 30% medications and 40% over-the-counter medications
- States with highest obesity rates have the greatest number of prescriptions written per capita
- Poly-pharmacy is a known risk factor for increased morbidity (illness) and mortality (death)
- Poly-pharmacy is responsible for up to 28% of hospital admissions and is the fifth leading cause of death in the United States
How does poly-pharmacy occur?
One can certainly debate the causes of poly-pharmacy, but as a practitioner in primary care let me list a few key reasons I see, especially in the United States.
- Poor nutritional status of modern American
- Heavy reliance on food pyramid which emphasizes high carbohydrate consumption & grains (Hence Obesity)
- Fragmented primary health care and reliance on specialty based health care**
- Patient attitudes and expectations that modern medicine “has a pill for everything”**
- Medical community bias against nutritional methods of treating illness
- Medical insurance model: Paying for sick-care rather than prevention
Role of specialty based health care
Fragmented health care, in my estimation, plays a role in the progression of poly-pharmacy. Hospitalizations and specialist referrals often lead to the addition of 2-3 medications but rarely ever removes a medication. Furthermore, one specialist writes a heart medication, another writes a stomach medication, and yet a third specialist writes a medication for the bladder or nervous system…so on and so forth.
Each specialist carefully avoids treating the “other” doctors area of expertise. Not wanting to step on toes, the predominant medical culture isolates responsibility for specific medical problems, medical-legally parceling out overall responsibility for care to no-one.
So what of the primary physician? Often primary doctors follow the same pattern. Instead of “owning” the entire patient’s health issues, they will select out less complicated issues and “assume” or delegate specific care points out to a specialist.
The result. Medications lists grown, complications rise, and health declines.
Patient Attitudes
The medical establishment does not shoulder the entire blame. I cannot lament the culture of medicine without focusing on the role patients play.
In over 10 years of clinical work in primary care, I will estimate 20% -30% of patients share a belief that the doctor “Has a pill for everything.” Naively, patients shift their own responsibility for healing and prevention to their doctor. The patient refuses to address lifestyle issues that cause or contribute greatly to their current medical problem.
This type of patient accumulates medications rapidly. One medication for the focal problem quickly becomes several as the patient returns to address side effects to the first prescription with…you guessed it….more prescriptions. (And the vicious cycle continues)
Curing Poly-pharmacy
I’m a physician, an MD. My “toolbox” includes the prescribing of medications to effect change and hopefully reverse the course of illness. I write about poly-pharmacy because I have daily reminders of the problem and risk this status has for my patients.
My practice has taken a different turn over the last 10 years as I have embraced nutritional concepts and better understood that true “healing” begins with my willingness to address prevention with patients. I also believe by sharing this message with those I lead, I can encourage others in primary care to “Own” the entire patient record.
Curing poly-pharmacy involves taking initiative, accepting the responsibility for removing medicines when they are redundant, contraindicated, or the problem–not the cure.
Curing poly-pharmacy also involves educating patients, especially the folks that believe cures come from pill bottles. Alerting them to the dangers of taking multiple combinations of medications simply to mask their lack of attention to fitness, balanced lifestyle, and nutritional choices.
Politics aside, poly-pharmacy is expensive in both dollars and lives. I hope you will share these thoughts with your friends, loved ones and health care practitioner.
I look forward to comments and examples of poly-pharmacy and outcomes from my readers.
I wish you were my doctor. I am a National Academy of Sports Medicine fitness professional with a specialty in corrective exercise. I see it so often. I train a more mature clientele and some of them will go to a physician for the littlest thing and sure enough walk out with another pill. I find it amazing that they don’t even change the dosage of the pill they were taking the time before. What’s even more amazing my client won’t even question it.
Thanks for the feedback Terryl. Culturally, a huge majority of Americans believe their health is not their responsibility. That’s not a slam, but rather a statement acknowledging that so often we look to a “Expert” to tell us about our own body. We also ignore mountains of research that very boring things like everyday fitness, nutrition, and lifestyle choices likely cause or prevent 80-90% of the medical problems treated today.
Keep up your important work! Best part of national healthcare legislation will likely stem from the pressure put on individuals to solve their own health issues….BTW http://www.Futurefocusmd.com is our home website….we do offer virtual visits…. (: